Advanced Scoliosis Care for Kids
The skilled, board–certified physicians at Children’s Orthopaedic and Scoliosis Surgery Associates provide the latest and most advanced treatment options for patients with scoliosis. Our physicians evaluate each patient carefully to determine the correct course of treatment for both surgical and non-surgical cases.
Children’s Orthopaedics utilizes the most advanced technology available to treat scoliosis, including minimally invasive surgical techniques and computerized intraoperative navigation. Our practice is affiliated with Johns Hopkins All Children’s Hospital and has repeatedly been recognized as Top Ranked Pediatric Orthopedic Care in Tampa Bay. Our three fellowship–trained spine specialists, Dr. Gregory Hahn, and Dr. Ryan Fitzgerald perform over 120 scoliosis procedures each year. Combined, they have over 30 years experience performing scoliosis surgery.
Additionally, our orthopaedic support team consists of knowledgeable professionals who assist our specialists in each step of the procedure, including pediatric nurses and patient care technicians with orthopaedic training, neuro–technologists, fellowship–trained pediatric radiologists, and pediatric anesthesiologists. Scoliosis treatment is often an ongoing process, and our goal is to provide the support and care that your child needs every step of the way.
What You Need to Know
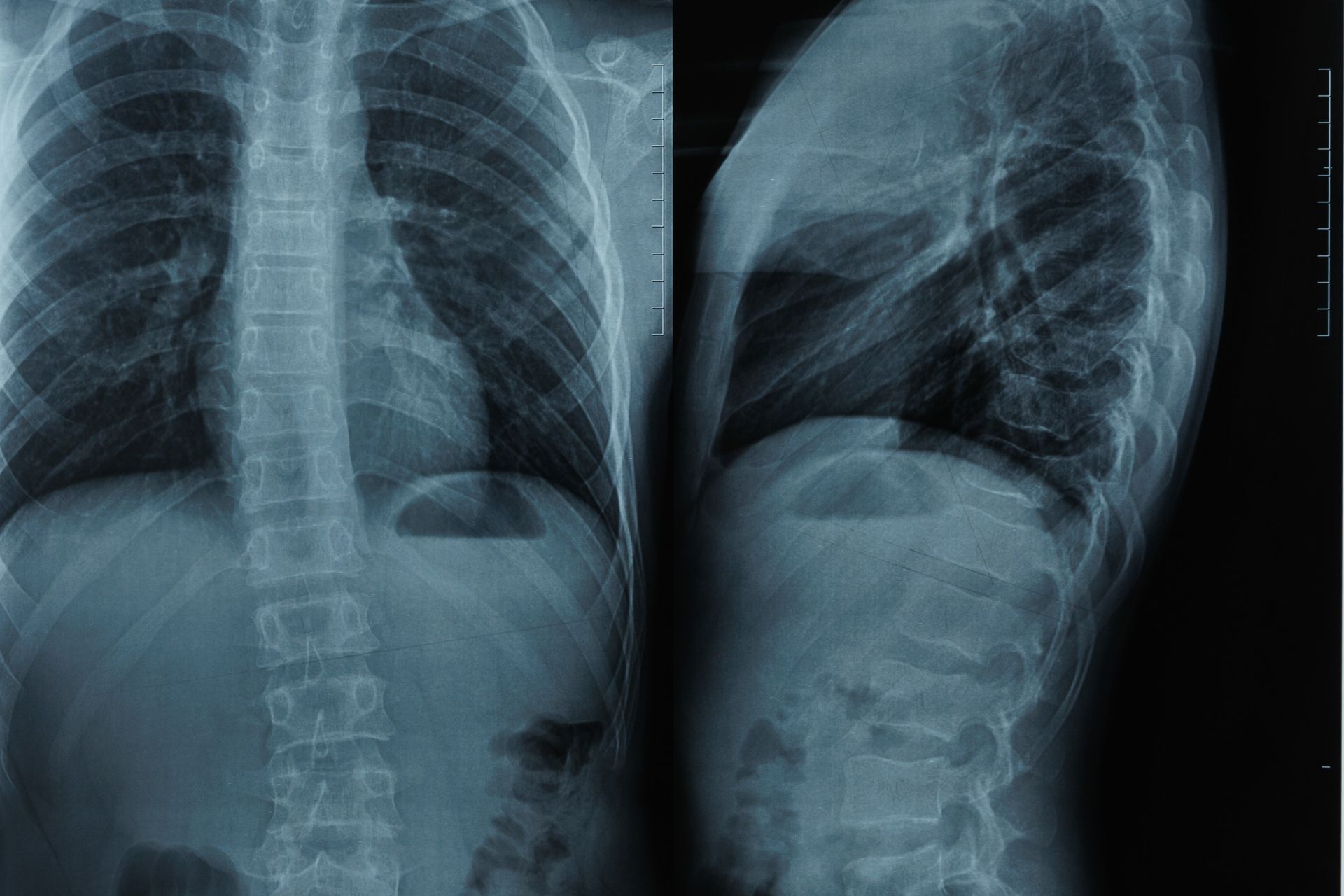
Scoliosis is defined as a side-to-side curvature of the spine. When looking at an x-ray of the spine in an individual with scoliosis, the spine may appear to have an “S” or a “C” curve. However, scoliosis is a complex three-dimensional deformity.
This condition affects approximately 7 million people in the United States, with the majority of cases occurring from age 10 through adulthood.
Early onset scoliosis (EOS) refers to spinal deformity or curvature of the spine in a child under the age of 10. EOS often occurs in patients with other health problems, including chest wall deformities, neuromuscular diseases, or spinal tumors. It is important for patients to receive a diagnosis and begin treatment for early onset scoliosis as soon as possible to achieve the best long-term results for the child. Depending on the severity of EOS, the child may also have heart and lung problems that can become life-threatening over time if left untreated. The goal of treatment for EOS is to minimize spinal deformity and complications, while maximizing lung function and motion of the chest and spine.
Understanding the Three Types
Congenital scoliosis is present at birth. This type of scoliosis develops due to a problem with the formation of the vertebrae in the embryonic stage of development. It is often associated with congenital fusion of the ribs, and may also be seen in conjunction with a number of other non-orthopaedic anomalies affecting the heart, kidneys, and gastrointestinal tract.
Neuromuscular scoliosis is caused by problems such as poor muscle control, muscle weakness, or paralysis secondary to diseases such as cerebral palsy, muscular dystrophy, spina bifida, and polio.
Idiopathic scoliosis does not have a known cause. Idiopathic scoliosis may occur at any age but is most commonly seen in adolescence. It may be genetic, running in some families. If it progresses, it usually does so most rapidly during puberty.

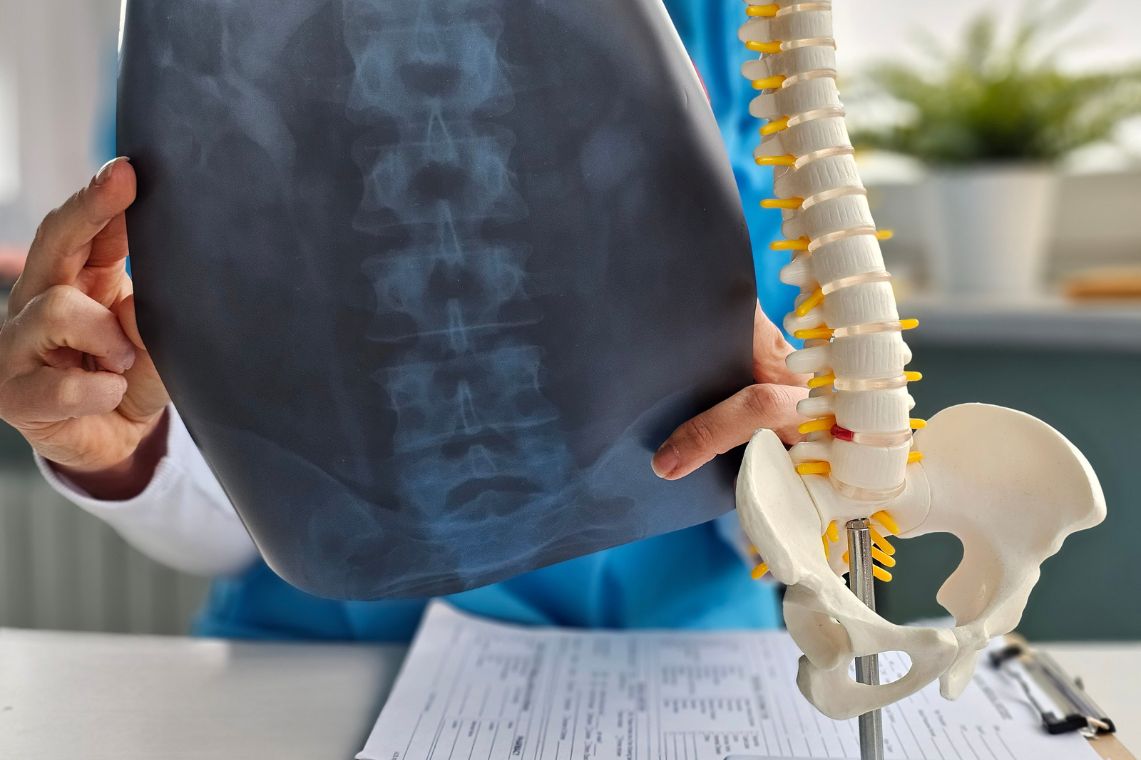
Identifying Scoliosis Early
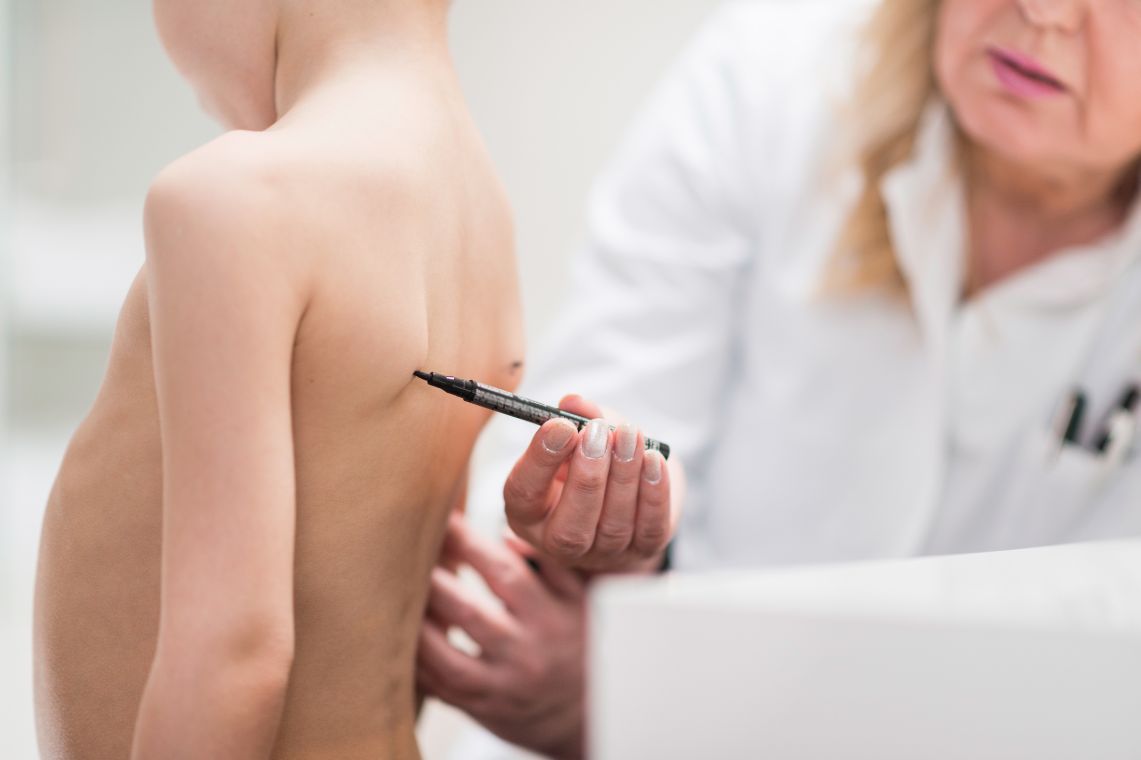
Scoliosis is usually painless. A parent or doctor may suspect scoliosis if one shoulder appears to be higher than the other or the pelvis appears to be tilted. Untrained observers often do not notice the curvature of the spine in the earlier stages. Children’s modesty causes them to avoid undressing in front of their parents. When the child is in a bathing suit, one may notice a sideways curvature of the spine or an elevation of one shoulder or hip.
During an examination for scoliosis, the doctor will ask your child to bend forward to reveal any rotational deformities. This is called the “Adam’s Forward Bend Test.” He will also check for any limb-length discrepancies, abnormal neurological findings, or other potential causes of scoliosis.
Exploring Treatment Choices
If your child has scoliosis, it is important to seek treatment. Without treatment, scoliosis can progress, causing functional issues and lower quality of life over time. There are different treatment options available, depending on the severity of your child’s scoliosis. Your physician will suggest the best treatment option for your child. Treatment options can include the following:
If it is a small curve, your doctor may recommend continual observation to check for progression as the child or adolescent grows. X–rays will usually be reviewed every 4 to 6 months.
Bracing may be recommended to prevent the curve from getting worse. Advances in orthotics and prosthetics have led to much more comfortable and lighter weight polypropylene plastic braces for scoliosis. In addition to the the foam-lined, body jacket-type TLSO (Thoracic Lumbar Sacral Orthosis) of the Boston type, nighttime–only Providence Braces have been shown to be just as effective for certain patterns of scoliosis. Experts continue to study the effectiveness of these newer braces in preventing progression of scoliosis. Unfortunately, no brace has been proven to actually improve scoliosis. That desired outcome is only available via surgical treatment.
Mehta casting is a great noninvasive option for very young patients with infantile idiopathic scoliosis. When Mehta casting is done early on, it has the possibility to “cure” idiopathic scoliosis. Even if it does not lead to a cure, it can improve the degree of the deformity and/or slow down the progression of the deformity and possibly delay the need for surgery. Children’s Orthopaedic & Scoliosis Surgery Associates now offers this treatment in conjunction with Johns Hopkins All Children’s Hospital.
Surgical treatment of scoliosis is usually reserved for curves that have progressed beyond 40 to 45 degrees. If left untreated, continued progression of these curves may lead to chronic, severe pain, deformity, psychosocial disability, and pulmonary dysfunction.
Spinal Correction Procedures
When surgery is indicated, our fellowship–trained pediatric orthopaedic surgeons offer the most advanced and proven techniques in reconstructive spinal surgery.
The surgical procedure used to correct scoliosis is called a spinal fusion. During this procedure, the surgeon will realign the bones in the spine and fuse them together using a bone graft so that they heal together into a solid piece of bone. Bone grafts may be taken from the patient’s hip, or an allograft may be taken from cadaver bone.
Our surgeons use different devices and technologies during the procedure, including pedicle screws, growing rods, and intra–operative image guidance.
Pedicle screws are used to anchor the correcting rods to the spine to prevent further movement while the spine is being fused with bone grafts. The screws are used to correct rotation as well as to treat deformity in the coronal and sagittal planes. The pedicle screws can be placed at multiple levels throughout the spine depending on the severity of the curve. The rods are then connected to the pedicle screws.
Growing rods are used to stabilize the spine in very young children with severe scoliosis, sometimes called Early Onset Scoliosis. The rods are placed through the muscles around spine spanning the curve and are usually attached with screws. Growing rods allow for continued, controlled growth of the spine in juvenile patients with scoliosis. The rods are then lengthened on a regular basis, approximately every 6 to 12 months.
Our operating room has been specially–outfitted with advanced imaging technology and specialized instrumentation to accommodate all of our orthopaedic surgical procedures.
CT–based, intra-operative image guidance allows the surgeon to navigate the spine using “smart tools.” The data from a CT scan of the spine taken before the operation is used to plan the procedure, including selecting the correct screw size and placement. These images are merged with real–time images of the spine during the procedure so that the surgeon has accurate reference points on where to place fixation devices.
This technology facilitates rapid and accurate placement of pedicle screws—there is virtually no chance of inaccurate placement. It also allows for more precise sizing of the screws within the pedicles and the vertebral body by allowing your surgeon to measure the pedicle and select the correct size. This reduces the chances of loosening or having the screws stick out from the bone.
Dr. Hahn and Dr. Fitzgerald utilize this technology very often in scoliosis surgery. Surgeons from around the world visit them at Johns Hopkins All Children’s Hospital to learn about these cutting-edge techniques.
Intra–operative neurophysiological monitoring helps protect your child from neurologic damage like paralysis. The goal of such monitoring is to identify changes in brain, spinal cord, and peripheral nerve function before irreversible changes occur. Motor and sensory monitoring of the spinal cord is conducted with every scoliosis procedure our surgeons perform in order to complete the case safely and efficiently.


Healing After Scoliosis Surgery
After surgery, your child will need to stay in the hospital for about a week. Following discharge from the hospital, your child will need to recover at home for about 3 weeks, on average. If school is in session, you may want to arrange for about 3–6 weeks of homeschooling with your child’s school.
During the recovery period, your child will need to avoid running, bending, and twisting at the waist. Your child must also avoid lifting anything heavier than 5 pounds. Full recovery can take from 6 months to 1 year, as the bones must achieve a solid fusion. After full recovery, your child can resume all normal activities, except for contact sports.
After scoliosis surgery, most patients will be able to function normally at the level they were prior to surgery. In most cases, additional procedures are not needed.
Our scoliosis specialists at Children’s Orthopaedic and Scoliosis Surgery Associates have extensive experience in helping children with scoliosis achieve a better quality of life. Our experts will help you through every step of the diagnosis and treatment process. If you think your child may have scoliosis and would like an evaluation, please call our office at (727) 898-2663 or request an appointment via our convenient online form.

Board Certified Orthopaedic Surgeon

Board Certified Orthopaedic Surgeon
What is Scoliosis/Kyphosis?
Meet our Surgical Team
Scoliosis Surgery Tips
Spinal Instrumentation and Intraoperative Computerized Image Guidance Video
Infants, children and teens with a wide range of challenging orthopedic problems benefit from the pediatric orthopedic surgery program at Johns Hopkins All Children’s Hospital. This expert care is provided by Children’s Orthopaedic and Scoliosis Surgery Associates…
